|
Care consultations help families avoid getting lost in the maze of payment options for elder care.
This blog series illustrate the ways a care consultation can save families money, time and trouble. These stories are drawn from our experience with families and their elders: identifying information has been changed. Paying for elder care is like making one’s way through a maze. In a maze, you can backtrack and take a different turn and it will only cost you time. In elder care, the wrong move can be very costly. Annie’s Mother was diagnosed with cancer and needed treatment. Following treatment, she was sent to a rehabilitation facility and then went home with help. All went well until she fell. The paid staff found her on the floor and sent her to hospital. Annie arrived to find her Mother in the ER. Tests showed she was dehydrated, poorly nourished and had not taken all of her medications. The hospital was overcrowded and so was the ER. Mother didn’t even get a room in the ER for 24 hours. The staff began treatments and Mother improved. Rather than sending her home, Annie decided it would be better to return her Mother to the rehabilitation facility. Annie also considered moving her Mother so she would not live alone to avoid future problems. This was especially important because Annie’s job took her all over the state. In an emergency, she might not return quickly. Annie didn’t review her Mother’s Medicare coverage. Mother had only been in the ER under observation. She had never been admitted to the hospital. Medicare covered many parts of her ER treatment. If her Mother had been admitted and had stayed long enough in hospital, she would have qualified for rehabilitation: she didn’t. Annie received the Medicare determination letter several weeks later: not covered. Annie returned her mother home, with more help, medication supervision, and more worry while she was on the road. She had to pay $18,000 to cover that stay. Consultations don’t cost, they pay.
0 Comments
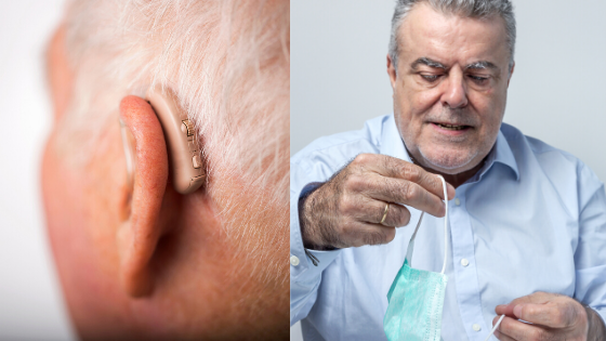
Covid-19 has required us to protect ourselves by wearing masks. Sadly, masks interfere with hearing aids. Thus, those who want to hear must contend with protection that makes hearing aids come loose, fall out of the ear, or tangled with the hearing device. That frustration could lead to quitting the mask or quitting the hearing aids.
We need both. Numerous research articles have documented the connection between maintaining one’s hearing and keeping one’s memory. Hearing aids are for more than hearing. On the other hand, the CDC guidelines are quite strict about wearing a mask to protect ourselves from Covid-19. We will need masks until we can develop an effective treatment and or a vaccine. That could be years. In Help! My Face Mask Is Getting in the Way of My Hearing Aid, AARP offers some ideas. While these might do for now, we should consider developing an easy-to-use, simple, device that does the job. If we can develop safety pins and zipper; we make a better device. Senior health studies show that social isolation is as important health as flattening the Corona-19 virus infection curve in seniors.
OPINION: It’s Time to Flatten the Loneliness Curve for Older Americans, by Marc Freedman and John Gomperts, was published in Next Avenue, April 20, 2020. The article discusses the impact of social isolation on elder health. This factor was an issue before Covid-19. However, the quarantine has made their social isolation even worse. The article references other countries’ methods of recognizing and responding to social isolation and encouraging elder social engagement. It offers several possible methods to facilitate the development of programs in the USA as engines to promote a better quality of life for seniors and for society in general. Did you know that grants were made last year to develop a Social Isolation Task Force and create a public education program? These grants were offered to all the state agencies that operate under the mandate of The Older Americans Act. I was on one of those task forces in my state. The assumption was the public wasn’t aware of the magnitude of social isolation amongst elders. Another assumption was the public wasn’t aware of the effects of social isolation on senior health and cost of care. Covid-19 changed all that. We‘ve all had a crash course in the experience of social isolation: the Stay-at-Home orders. We’ve seen people reacting, sometimes threatening violence, in a push-back against such measures. Children have suffered socially, emotionally and in their education as a result of being isolated from friends and school. To combat Covid-19, social isolation was one of the few measures we could employ. While we intended to combat the virus with isolation, we didn’t intend to isolate elders before Covid-19. Our society’s systems just didn’t address elder social isolation. Our society did not face social isolation before because of three factors; our original population, our history, and our lack of a collective memory experience. Our population was largely imported, usually young adults and their children. Later, they might send for the elders in the old country, or not. A sea voyage could be quite stressful on an older person. Thus, young people settled here. Later, another generation of young people left for the next new frontier. Our history shows that elders were left behind; again, and again. As a result, our focus was a succession of new frontiers. The USA never developed a role or task for elders. Today, our old frontier is closed. It’s time to bring society into the new social frontier: one in which we recognize we are a multi-generational country. There are gifts from each generation. We need to develop a role, and a function that recognizes the value of elders: a living history, perspective and experience. We also lack a collective memory of the elder’s journey. We all remember things from our childhood; many of us may not “remember” things from our elder hood; unless we have made that journey ourselves. Society hadn’t experienced certain aspects of aging, like social isolation, until now. We should view stay-at-home orders as our chance to learn what life is like for seniors who are forced to stay-at-home. What puts elders in that position? Their health may not permit frequent trips outside the home. Other elders are trapped at home because they can no longer drive. Public transportation may be too infrequent, too strenuous, or non-existent. Some elders find that vision or hearing problems interfere with socializing. We have few forums in which all generations come together. Religious institutions fill some of that gap but they can’t cover all the bases. Our neighborhoods are often age-segregated. Schools group children into smaller age cohorts: this is not the era of the all-ages, one-room school house. We build age-segregated housing only for elders. How is anyone to learn about the elder journey if our opportunity for observation and interaction are taken away? Covid-19 has given us a gift in disguise; we all shared some of the elders’ social isolation predicament. We reacted vehemently to these restrictions on ourselves. Now we know what they feel. The recommendations made in this article should be implemented. Let’s learn from this. As the old song says; ”Someday, some d-a-a-y, we’ll be together. Yes we will, yes we will...” Has this happened to you? “I took groceries to my Mom. She wanted have coffee with me. I’ve tried to tell her I couldn’t, but she just doesn’t get it! I don’t know what to do”!
Caregiving is a demanding process and Covid-19 adds more demands. Caregivers still try to respond to their loved ones even under new circumstances. In the past, the caregiver could might take the elder shopping; not now. Shopping was an outing, a chance to socialize, and a chance for the caregiver to assess how the elder was doing. Now, we wear masks and are encouraged to shop as quickly: a-l-o-n-e. We only have a fleeting glance at our loved one on food drop-off. We can’t just pop in the house or care facility to check on things for ourselves. We must rely on reports from our loved one, the staff or (sometimes) the news. Imagine reading the news and learning your parent’s facility has a Covid-19 outbreak! Caregivers revealed they felt guilty before, it’s especially true now. Some guilt seems to be rooted in the feeling, “I can’t do anything!” Yes, you can. Caregivers used to worry about elders taking medicine properly or eating regularly; now worries include possible exposure, illness & death. To add to these concerns, seniors seem to want more from the caregivers. They ask caregivers to run more errands or ask for things not appropriate to their diet or welfare. An elder asked me to try to take money out of an ATM with his bank card! Why are elders making more or different or even illegal requests? There are a couple reasons. First, caregivers make the distinction between the Covid-19 as the cause and the changes in our lives as the response. Sometimes, that distinction is not as clear to the elder. “They just don’t get it”; is a sign to caregivers that the senior hasn’t understood in the first place. Everybody has studied something that felt very different when actually experiencing it. Think of your first time behind the wheel of a car. No instruction manual prepared you for that feeling of your foot on the accelerator. Childbirth classes help, but they can’t communicate what it feels like to give birth to a child. After the experience, we “got it”. Making it real,related to the senior’s early experiences, helps them to “get it”. Second, caregivers understand the impact of this pandemic process. So, instead of doing more errands, we need to take the time to help seniors grasp the process. We feel guilty because we can’t take them out, or can’t give them a hug. So, when they ask for more and more, we do it because it makes us feel better. Have you noticed that more errands just aren’t enough? That’s because errands don’t fill the senior’s real need: finding meaning and support. A conversation, in which you focus on their early experiences, such as quarantine, helps them feel the reality of current circumstances. Explanations don’t work as well as a trip down memory lane. Just making the effort to help them understand the experience will fill their need for direction and support from you. Your senior relies on you in ways they can’t express. When they feel like the world has gone crazy, they look to you. When you show effort to help them understand (not expertise) they become calmer and you’ll feel better too. Third, just saying NO, puts limits into their lives and is another way to calm your senior. When times are uncertain, a clear guide creates a sense of stability. They sense that you are looking out for them and you are their leader through these times. Your firm guidance gives them clarity. Then, you have more time and the emotional space to feel less guilty. Caregivers need not do e-v-e-r-y-t-h-i-n-g; just the right things. Fourth, a rule of thumb for elders with dementia is; the more dementia, the longer “emotional antennae”. Your seniors are highly attuned to your moods. They just can’t process the information the way they used to. Covid has shifted everyone’s life. Elders sense that you are struggling to adjust your lifestyle. Caregivers may not want to show these struggles. They feel guilty these the elders depend on their care. The elders already know. When you put words on your feelings, it’s like putting on an oven mitt; now you can handle hot stuff. Your words become the elder’s way to express their own feelings. Keep it simple but keep sharing. Remind them of any major adjustments they had to make in the past: WWII rationing, Great Depression job losses. Emphasize how they made it through hard times and the example they were to you. Thus, the caregiver becomes the mirror that reflects the senior back to their best self. Finally, remind the elder this is only for now, it will not last forever. As the old song says: “Some day; s-o-m-e-d-a-y, we’ll be together (yes we will)! A daughter commented that she had not been able to visit her parent because the facility was “locked down” to prevent the viral spread from Covid. She could only drop his snacks off at the door. She worried. No matter how many times she explained, she still couldn’t get him to understand. Many elders and their adult children face this dilemma. All facilities are closed to visitation: even when the elder is dying! The more frail the elder, the less likely they can manage total separation. Seniors need tangible connections; touch, sight and hearing. How do we keep in touch in an era of no-touch? Families often bring presents to these visits, yet; it’s the present of their presence that elders crave. So, how do we convey presence when we can’t be present? KEEP IT TANGIBLE: E-cards are nice but a classic greeting card is tangible.Your loved one can hold it or look at it repeatedly. Tuck a greeting card into a bag of groceries or a bunch of flowers. The facility staff can point to it to remind them that you are keeping in touch. MAIL CARDS: It helps support our postal service and your loved one. Getting mail is a big event in care facilities. It’s not how fancy the card, it’s how often you provide a reminder that you care. TRY PRINTED PHOTOS: These are more tangible. Perhaps you got your loved one a cell phone and sent them pictures. That wasn’t their early experience. For decades, today’s elders only had the paper option. When you send a shiny paper photo it resonates. Photos used to require going to a studio, posing, and were made for special occasions. Photos were important. So printed photos carry an important message from you; “You are important to me”. Children’s crayon drawings carry the unique, tangible message. They are especially important if the drawings are labeled with the child’s name, date, and something about the picture. That way, the staff can point out the picture later, when the elder says they think they’re forgotten. WHAT’S THEIR FRAME OF MIND: We’ve all had a crash course about pandemics. Elders may not have paid as much attention to the news. Some have turned news off altogether. 98+% of today’s elders weren’t alive during that last pandemic in 1918. It isn’t part of their experience. They can’t relate to the scale of lock down necessary to contain a pan-demic. Some may have known families who were quarantined when they were children; but they are not familiar with a whole society in quarantine. So what do you tell them about why you can’t be there? Start by asking them what they know about today’s news. If they have been following the news, use their level of information to determine what you share about your being away. If they don’t seem to know; try a simpler explanation: you “have to be away for awhile”. You’ve taken vacations, trips and returned. This is just another time away. Promise only that you will return. Say that in a card as well as on the phone. Say it often. “ Someday, some way, we’ll be together”. That’s what the song says and that’s my prayer for all of us. Corona Virus-19 is not your parents' quarantine. Before vaccines, quarantines were a common event. Your senior may have lived through several of them. with the passage of time, the anxiety and social disruption may have been lost. All that remains in their minds is that they survived. I've met some seniors who think this is just another flu. They believe that, because they've lived this long, they're immune. It's been a challenge to convince them that this virus has an impact closer to that of the 1918 Spanish flu. I usually ask them if their parents ever discussed the Spanish Flu. Then I draw the comparison.
I've also had to explain that our immune systems change with age. We all know hair turns white/gray with age but not all changes are equally visible. The senior may not realize that they may succumb to this disease because their immune systems are affected with age. I share these points to forewarn caregivers that your senior my see this disease very differently than you do. What's in your senior's mind? If the senior doesn't get the message, they will be more likely to get the disease. Stay well and set a good example; wash your hands with your senior. Thanx, Sara The Strange Psychology of Stress and Burnout, which appeared in BBC WorkLife’s November 17, 2019 post, discusses the relationship of stress to Cortisol; important. The article described several results or diseases that begin with exposure to prolonged stress. It also mentioned some situations that can cause stress but left one out; caregiving! Already, 34.9 million people are self-identified caregivers. In addition, some people are starting to do caregiving and don’t realize they’re in this new role; yet.
This article shows the photo of a man; yet 66.5% of caregivers are women. The photo shows multiple phones. Yes, many caregivers have spent time on the phone to coordinate care for the elder. However, caregivers face the competition of simultaneously dealing with home, job, and possible child care while doing caregiving! The focus of the article is on job-related stress. Caregivers bring their stress to work with them. Thus, what looks like job burn-out might be a result of simultaneous stressors; job and caregiving. The remedy described in the article involves changing the perception of the person under stress; Cognitive Behavioral Therapy and changing jobs or shifting responsibilities. Sadly, these are not usually available to the family caregiver. She may not have insurance coverage for therapy. Group insurance plans may not recognize family caregiving as a stressor worthy of intervention. How does the working caregiver access therapy? She has no “off-duty” time. She goes from the career job over to the home “job”. It’s time for all of us to make sure caregivers as SEEN and heard. “‘This will be catastrophic’: Maine families face elder boom, worker shortage in preview of nation’s future,” from The Washington Post, could be a description of a dystopian movie: it’s not. This is the state of State of Maine, which is the harbinger of things to come for the rest of these 50 United States. We need to listen to this alarm.
We’re facing a demographic dilemma: not enough young people to fill all jobs, even those outside of elder care. We need them now! Where do we get them? We can’t hire them because they were never born! Thus, current workers remain on the job long after it’s safe or appropriate. Results include accumulated injuries to workers who keep doing injurious jobs. Even the field of healthcare can’t find enough workers or volunteers. The State of Maine has learned that there is no one available to fill home care jobs. There is no one to fill care facility jobs either. Professional fields have the same problem; many of the number of nurses and doctors are now older and there are not enough of them it is and there’s no one to replace them. Medicaid pays far less than other employers, drawing the few workers away from elder care. However, simply raising wages won’t help if there are not enough people to hire! Maine is already experiencing the results, some facilities closed altogether. Others closed admissions for months due to too few staff. No vacancies in care facilities means families must place their loved ones wherever they can. A loved one far away means a l-o-n-g commute to visit. Younger, disabled people also get caught in this care-crunch. If no one is available, some adult children try to fill the gap. Those care gaps further pressure the few remaining working adult children. Keep this number in mind: *By 2030, 1 in 5 Americans will be over 60. *The number of seniors will DOUBLE between 2015 and 2050. *The senior population over 85 will TRIPLE in that same period. **We will need 7.8 MILLION new people to fill these jobs. Since we didn’t give birth to them; where do we get them? This isn’t as riveting as a news story as a fire, or a shooting, that’s the problem. The numbers of affected families are there, but they aren’t collected (aggregated). This problem is spread everywhere. We’re in a presidential campaign yet no candidate is talking about this national problem. Why? This demographic dilemma is happening one family at a time: Your family is next. The Reuter's article, U.S wages lost to unpaid family care to hit $147 billion by 2050, describes lost wages and pressure on caregivers to switch to part time work or quit all together. These are definable numbers which the article describes well. One doesn’t hear enough about these issues and costs in the news media. I call upon anyone who knows a caregiver to insist on better public discussion on these caregiving issues/ costs/pressures.
I've always worried that caregivers also lost opportunity as well as wages. They are less likely to be offered new projects at work which can polish one's resume. They can’t take the lateral move which puts the employee in line to move up in a branch of the organization. A promotion comes with more demands on time and a different schedule. How can the working caregiver manage that? Promotions may mean a move out 0f town; how does a caregiver juggle that? So less chances to rise in a career. In addition, caregivers suffer hidden damages to their careers. Just taking repeated PTO (Paid Time Off) casts a shadow over one's career. Eventually, PTO runs out. When PTO runs out, the employee is left with FMLA (Family Medical Leave Act). That is usually unpaid. The employed caregiver must consider loss of income along with caregiving pressures. I'm also a member of Society for Human Resource Management (SHRM), and read their daily dispatches. It appears that employers are more comfortable allowing the employed caregiver a block of time, like a week or two, to handle a health crisis. Piecemeal time tracking is another matter. There are some tracking systems, however, these seem to be evolving methods. The employed caregiver may need to use her time in piecemeal form. Perhaps she takes her lunch time to supervise the elder taking medications. Her commuting time would be deducted from PTO or FMLA That's the typical shape of elder caregiving, a mosaic of times and tasks squeezed together throughout the day. So both the employed caregiver and her employer are both carrying this process. The caregiver is doing the tasks and the HR manager is handling the administration. This produces an implicit time cost to the employer. Why would the caregiver’s boss consider her for special projects, a move, or a promotion? These would demand more of her time and the employed caregiver doesn't appear to have any time. In order to develop one's career, one must appear to be ready and willing as well as able. No employer really knows whether any employee is truly available. However, a string of PTO/FMLA requests create an image of less availability. It’s a subtle form of job “loss” that doesn’t show on the paycheck. Only the US and England have a patchwork-to-none system for dealing with our aging population. Other European countries have created caregiving support systems. Why aren’t we looking at them? According to The Strange Political Silence On Elder Care, the problem is our society has an extraordinary number of caregivers who haven’t formed a group to push for change. Unlike other groups, such as Mothers Against Drunk Driving (MADD), caregivers should have formed a constituency to insist on changes which better support them; but they haven’t. Why not? One surprising finding is that caregivers don’t recognize themselves! How can our society offer support to a person who denies needing help? How can we help if they believe they can’t ask? What is the effect of this lack of coalescing, lack of self-identification and the resulting failure to prepare and plan?
This article describes the possible reasons:
Senior Sidekicks has stood with caregivers for the past 12 years! The caregiving phase is the newest part of life’s journey. A little over 100 years ago, people didn’t live long enough to reach this stage. Our firm has struggled to get new caregivers and those in the midst of caregiving to accept help. Perhaps this article explains why people, who are otherwise prudent, take such a strange view of caregiving. Let’s compare and contrast caregiving attitudes with attitudes to other parts of life’s journey: Your getting married, do you make plans? What kind of a wedding would you have if you didn’t acknowledge you were engaged? How would you bring your lives together in marriage: legal, financial, religious, integrating your families, where to live, and children? My parents, like many during WWII, had a hurry-up wedding. They were high school sweethearts, and engaged in college. When my father finished his course work and ROTC, he was shipped to Texas. The university mailed his diploma. My mother took the train to Texas and they were married by a preacher on base. They had 3 weeks of wedded bliss before he shipped out for 3 years! Mother went home to a fire storm! Both sets of parents were in shock. Mother had not completed her college education; could she go back and finish? Would the all-girls school take her back as a married woman? Neither of my parents had completed paperwork naming her his spouse? Forms and letters took a long time to reach soldiers in the field and even longer to receive replies. Who would be the listed next-of-kin in the event he didn’t come home? She even had to discuss possible burial arrangements!! Who was now responsible to pay for her education? Was she to receive his pay since she was his spouse? Mother described it as a very trying time that she had to face alone because they didn’t plan. Weddings are as much a family matter as caregiving. A wedding, without planning, causes major stress. Caregiving, without planning and support also causes major stress. Yet, families will tell me they’ll handle it all by themselves: really? Let’s look at another example: You’re having a baby! Does that mean you don’t need any help? If you’re expecting do you still need proper medical care, resolve legal matters, insurance, or a larger place to live? We expect that expectant parents need help. We’ve developed the social systems to provide it. Having children brings many resources into the family. There are Family Medical Leave Act (FMLA) for both parents in certain situations. There are prepared childbirth classes, visiting nurses to the home after delivery and new mother’s groups. Relatives come to help the new mother and baby. Everybody sends food! It’s acceptable to have help for babies, why not for caregivers? The difference is we’ve had babies for millennia; caregivers, less than 100 years. Thus, the family caregiver may or may not receive some defacto help from her church, neighbors, or friends. There’s no visiting nurse system. The caregiver can take FMLA but it’s complicated and doesn’t always cover the type of caregiving the employee needs to give the elder. Many FMLAs don’t pay the employee. Caregiving may mean moving the elder closer to the caregiver, or moving in with the elder. Caregiving may be so demanding that it afflicts the caregiver’s health. The caregiver may be forced to quit the job. A break in the caregiver’s career creates a major financial setback as the caregiver tries to re-enter the workforce. Caregivers often draw on their retirement savings during caregiving. Other developed countries have seen this writing on the wall and started putting plans in place. Why can’t the US do that? We can, if we act now. You can do two things:
Talk to your neighbors. Ask what your church is doing for caregivers? Ask your employer the same thing. FMLA, by itself, is not an adequate response.) Are you a member of a union; put caregiver support on the bargaining table. We already have mandatory courses in sexual harassment and discrimination. Make caregiving training the next mandatory course. Are you an employer? If you prepare for tornadoes; prepare for this gray tsunami. By 2030, 1 in 5 Americans will be over age 60 ENTER THE POLITICAL DEBATE ON THE SIDE OF CAREGIVERS: It’s time to insist that the political conversation of this campaign is about p-r-e-p-a-r-i-n-g for this gray tsunami! It touches everyone. It’s not red or blue, it’s GRAY. Candidates will ask for your vote; tell them to put caregiving in their platform to get your vote! Caregiving is at least as important as any other policy |
Author "A Senior Moment" is written by Ms. Sara Lieber, owner of Senior Sidekicks. Ms. Lieber has over 30 years of experience in senior care. Archives
March 2024
Categories
All
|










 RSS Feed
RSS Feed